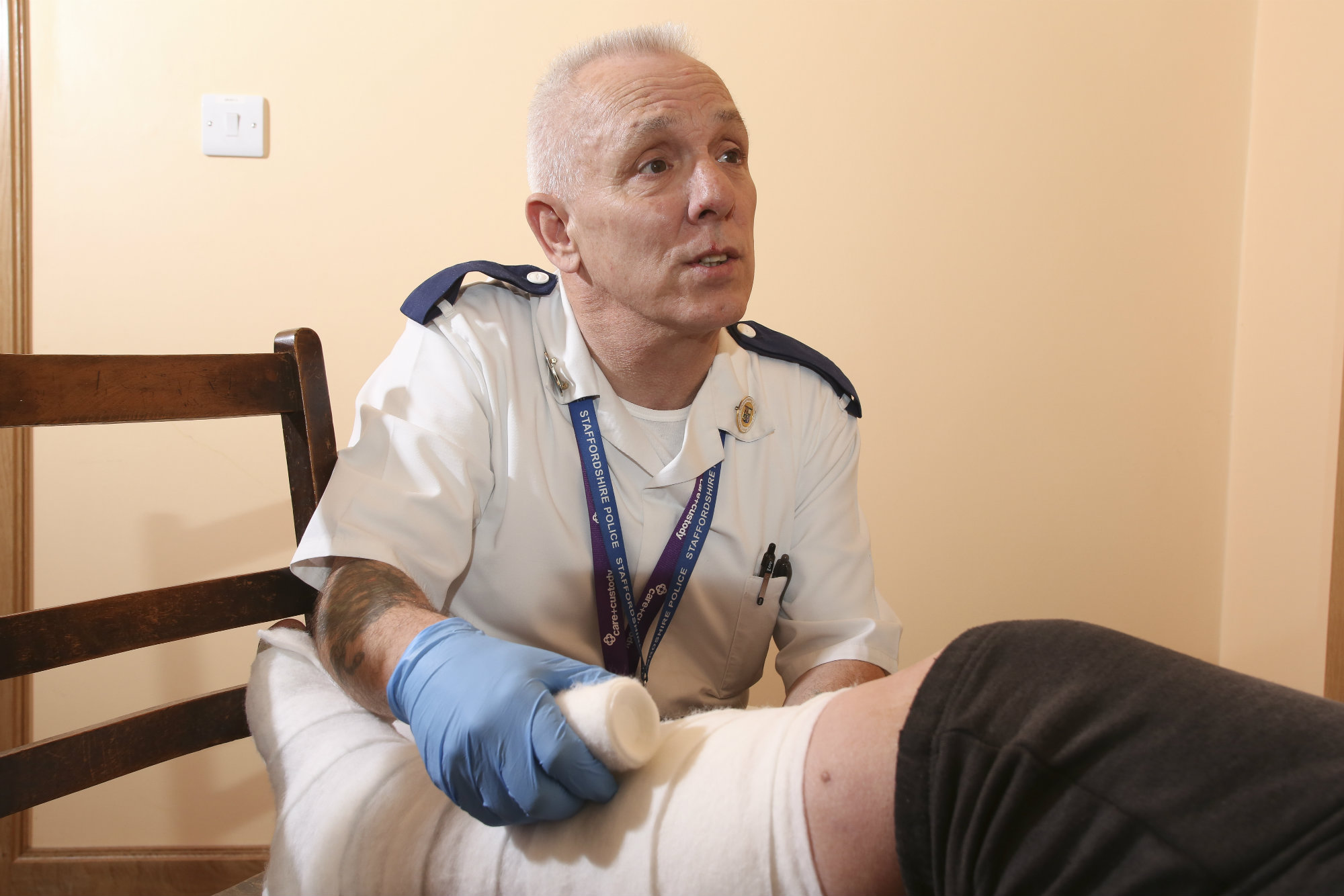
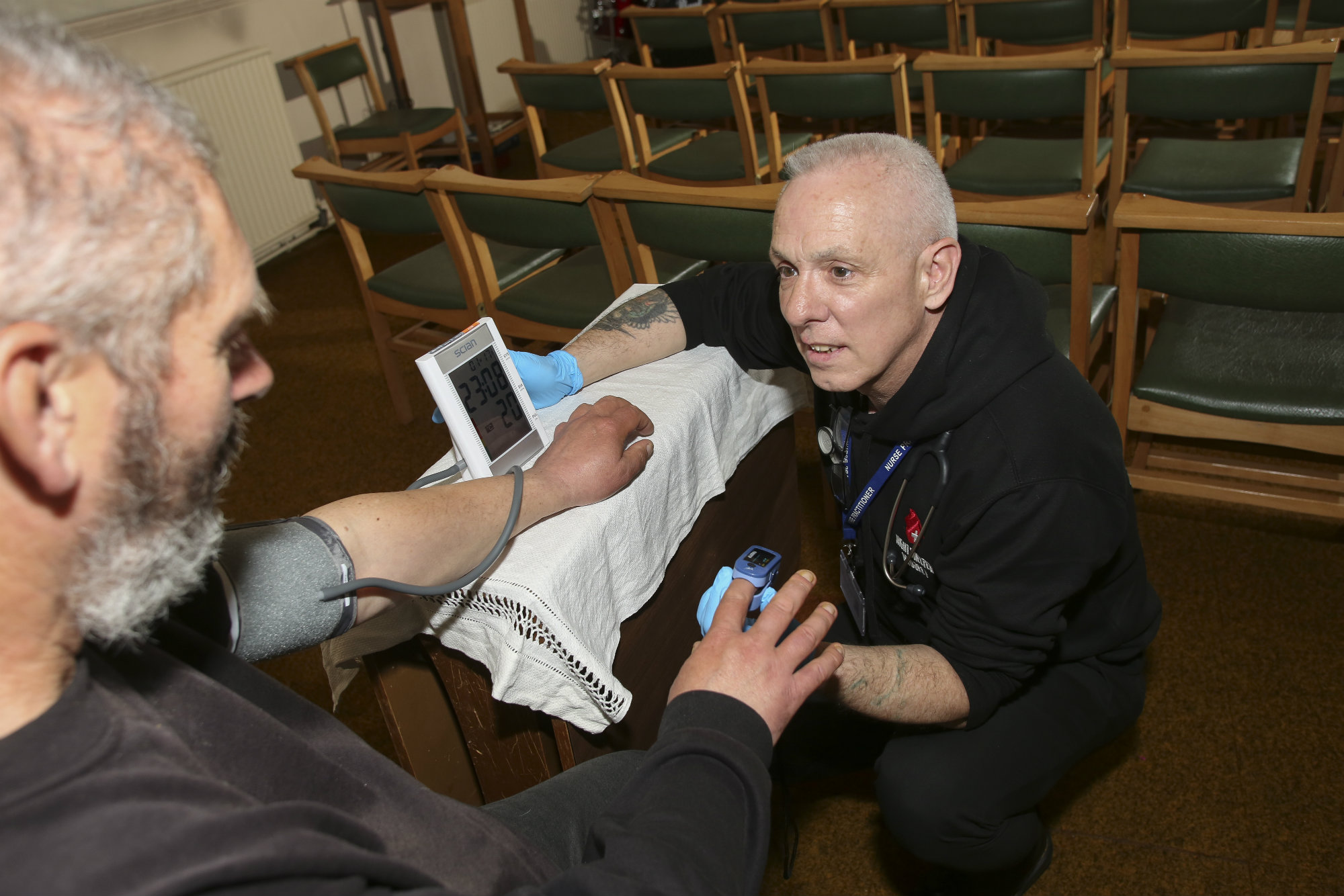
For forensic custody nurse Eric Teague-Hellon, watching the same people be detained time after time inspired him to try to change their lives. His impactful work has now been recognised with the RCNi Community Nursing Award.
“We see the same faces return two or three times a week,” says Eric, who works at Staffordshire Northern Area Custody Facility. “The majority are homeless and often they’re committing low-level crimes, such as shoplifting or minor damage, just to get a warm bed and food for the night.”
Alcoholism and intravenous drug use also take a huge toll on their health. “They have a lot of chronic illnesses that they don’t get treatment for, including asthma, diabetes and skin ulcers,” explains Eric, who is a member of the RCN Nursing in Justice and Forensic Health Care Forum and has been working in this field of nursing since 2009.
“They may even have life-threatening conditions, but if we try to send them to A&E, they either flatly refuse to go or won’t wait, because the drug and alcohol withdrawal symptoms take over. Their health just gets worse and worse.”
Knowing that they wouldn’t use mainstream services, Eric decided to take health care to them, with a range of initiatives. These include visiting local night shelters, in his own time, where he offers assessment, check-ups and treatment; providing food bank vouchers for those in crisis; and taking out hot food to the rough sleepers.

Remarking on the RCNi Community Nursing Award, Eric said: “I am so pleased. It’s helped me spread the word to a much wider audience, with nurses contacting me and wanting to help, and others giving donations of food and clothes.”
Since he started his project in earnest last September, another couple of nurses have joined him in the outreach work. Now if he advises one of his patients that they need further hospital treatment, a volunteer accompanies them. “They feel more secure and that they won’t be judged,” says Eric.
You don’t want to watch someone deteriorate when you have the skills and knowledge to stop that happening
He has also found that a high proportion of consistent offenders are no longer reoffending. “They are getting what they need in the community,” says Eric. “It’s amazing to see the results. Having been through a very harsh winter, we’ve managed to keep everyone going. We’re gearing up now for next winter, collecting sleeping bags and warm clothes.”
Looking ahead, Eric’s ambition is to roll out his project to every UK custody facility. “It only takes one nurse in each place to make a huge impact on our most vulnerable,” he says. “As a nurse, you don’t want to watch someone deteriorate when you have the skills and knowledge to stop that happening. When I visit someone, I don’t see a drug-user or a homeless person, but someone normal and a friend, who for whatever reason took a wrong turn.”
Three more forum members were also honoured at this year's awards for their leadership and innovative work:
Putting patients at the centre

Patients who have cancer with an unknown origin often face a variety of difficulties, including complex care journeys, numerous investigations and lengthy hospital stays.
Now a team at NHS Lothian, led and developed by RCN Cancer and Breast Care Nursing Forum member Gillian Knowles, is helping these highly vulnerable patients have a much better quality of care. Their work has been acknowledged with the RCNi Cancer Nursing Award.
“It was lovely for our team to be nominated,” says Gillian, who is a nurse consultant. “And I’m delighted that our work has been recognised. As the first team in Scotland to develop a service for these patients, who were not well-served in the past, we’ve worked hard to make their experience better. It’s a great accolade for our organisation too. There are many positives.”
Before the service began, these patients could often fall between different departments, but now there are developed pathways for diagnosis and treatment. Audit shows reductions in the length of hospital stays and the number of invasive investigations, alongside improved and timely support and cost savings.
“Often these cases are not straightforward, so patients could bounce from team to team in an attempt to find the primary cancer, but it was not the right way,” says Gillian. “Essentially our service puts the patient at the centre of their care.”
Driving change

While research has traditionally not had a high profile in emergency departments, Professor Heather Jarman’s award-winning work is challenging that situation.
“It struck me while I was doing my own research that there weren’t the opportunities for staff and patients to take part,” says Heather, of St George’s Hospital in London. “While there’s a huge number of patients who could take part in studies, it’s not thought of as an environment where it’s possible.”
But thanks to her hard work and perseverance, four years later the hospital’s emergency department has a thriving and highly regarded research unit - and now Heather’s contribution has been recognised with the RCNi’s Emergency Nursing Award. “I’m thrilled,” she says. “My team did it secretly and I didn’t know until I got an email saying I’d been shortlisted. Winning is amazing. But you never do these things alone and we’ve all worked so hard to get to this point.”
A former vice-chair of the RCN Emergency Care Association, she believes that being offered the chance to take part in research should be routine for both staff and patients. “That’s my big drive,” says Heather. “We see 160,000 patients a year and I’d like to see every one of them being able to participate in a trial, if that’s what they want.”

Yvonne Manson, Older People’s Forum member and winner of the RCNi Leadership Award, talks about her work:
"I have a passion for dementia care and, having worked in care homes for 23 years, I want to remove the stigma associated with working or living here, highlighting the positive nursing career and innovation that can be achieved.
"I work as a nurse consultant in dementia for the Balhousie Care Group in Scotland, which supports more than 700 people with dementia or cognitive decline. To be able to provide the highest standard of care, I developed a strategy, visiting all 25 homes to gain the views of staff, residents and their families.
"It was no simple task as our care homes are spread throughout Scotland - including Aberdeen, Arbroath, Perth, Dundee, Fife, and Kinross. Building trusting relationships meant visiting as often as possible. But when the programme was finally agreed, gaining buy-in was easier. As everyone had been involved, they willingly signed up to support it.
"Education is a key aspect of our strategy. So far, our training programme has been completed by more than 600 staff and family members. We also evaluate the impact of our dementia services regularly and since the programme began, mood and engagement scores have increased. In addition, we have increased our original team of four dementia ambassadors to more than 90.
"Overall the strategy has had such a positive impact that it has been shared widely, outside our organisation too. I regularly get emails from people who have read about it, asking how they can put something similar in place."
Find out more
Read more about the RCNi Nurse Awards and the winners from this year at www.rcni.com/nurse-awards.
To see the full list of RCN specialist nursing forums and join, visit www.rcn.org.uk/forums.