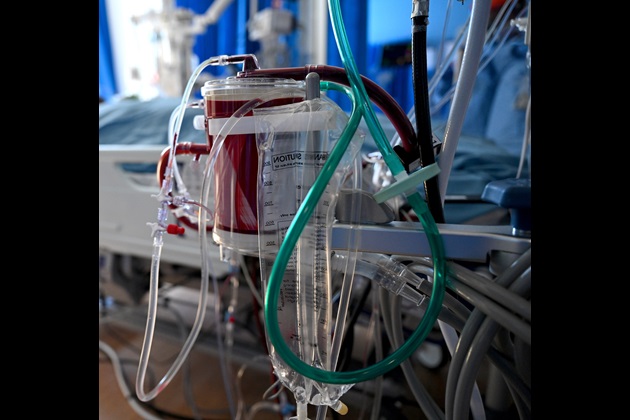
Nurse consultant Jo-anne explains how this lifesaving technology is being used to oxygenate the blood of people with severe COVID-19 symptoms, allowing their lungs to rest and heal
Specific patients in specialist intensive care units are being supported with extracorporeal membrane oxygenation (ECMO), a medical support delivered continuously at the bedside.
Jo-anne Fowles is an ECMO nurse consultant at Royal Papworth Hospital in Cambridge, one of only a few hospitals in the UK offering the service.
ECMO is a technology that has helped patients with severe respiratory failure, including when that’s due to respiratory viruses such as swine flu (H1N1) in 2009 and again now with COVID-19.
How it works
In severe cases of COVID-19, the virus can cause a patient’s lungs to struggle to ventilate, unable to add oxygen and clear carbon dioxide, and that’s where ECMO comes in.
It doesn’t treat the patient’s underlying illness but supports the lungs while conventional therapies are used to treat them, or time is given for natural recovery processes to kick in.
A patient’s blood is removed from the body, usually from a large vein in the neck or groin, then passed through the ECMO machine. There, carbon dioxide is removed from the blood and oxygen is added before the blood is transferred back into the body.
“It acts like the patient’s lung outside the body,” Jo-anne says.

ECMO is administered to patients who have a reversible severe lung injury and is usually used for conditions such as very severe asthma, severe pneumonia and acute respiratory distress syndrome (ARDS). It allows a decrease in the degree of injury caused by mechanical ventilation.
“In cases of very severe asthma, when it is often extremely difficult to use a conventional ventilator without damaging the lungs, ECMO is a really good support,” says Jo-anne.
“We can put ECMO on for a short length of time for these patients to support their oxygenation and carbon dioxide removal while treating the severe asthma attack.”
It acts like the patient’s lung outside the body
Putting a patient on ECMO is decided collaboratively between the referring hospital and the ECMO teams, and it depends on specific guidance, clinical criteria and advances in understanding where it can be beneficial to patients.
“The national ECMO service is not just about Royal Papworth, it’s about the five centres in England working together. Other centres have also joined the service during the pandemic to add capacity,” says Jo-anne.
“We work as a multidisciplinary team with medics, perfusionists, physiotherapists and nurses in different roles. We try and keep it patient centred,” she says.
The nursing role
Jo-anne’s unit has had to make changes to meet the challenges of the pandemic. It has been treating COVID-19 patients since March last year.
Having helped develop the role of the ECMO nurse specialist at Royal Papworth Hospital – with a bespoke training programme including study days, assessed reflective essays and clinical assessments – Jo-anne has been well-placed to organise the unit’s response.
Nurses in ECMO units have two responsibilities: they provide bedside care and they monitor the ECMO machine. “As a bedside nurse, we do all the things you would do for any critically ill patient,” says Jo-anne.
“If we’re talking about COVID-19, normally an ECMO patient would have a nurse on a one-to-one ratio, but sometimes we’re having one critical care nurse to two or even three ECMO patients. However, we always maintain safety and a very high standard of care for our patients.”
To help meet demand, redeployed nursing staff, doctors and allied health professionals have taken on the role of bedside caregivers, freeing up the ECMO nurses to manage the equipment for several patients at once. “It’s a team approach which means we can offer this support when there are so many patients,” Jo-anne adds.
We work as a multidisciplinary team with medics, perfusionists, physiotherapists and nurses in different roles. We try and keep it patient centred.
Supporting recovery
Patients are liberated from the ECMO when they show signs of recovery. They’re monitored as ECMO is turned down to minimal support, and if this is successful, a trial of no ECMO support is carried out.
If the patient can tolerate this for 24 to 36 hours and maintain their own oxygenation levels, the support is removed. Afterwards they are cared for like any other ICU patient.
Some COVID-19 patients are staying on ECMO for much longer. “The average length of time for our patients supported on ECMO has always been about 14 days. During the first surge, the average time for our patients on ECMO supported for COVID-19 was more like 30.”
It’s a team approach which means we can offer this support when there are so many patients
One of Jo-anne’s surviving patients was on ECMO for more than 60 days. “We assess our patients continuously – and every patient is very different,” she says.
Just like other intensive care staff, nurses on the unit have had to adapt to the challenges of wearing full PPE, undertaking procedures such as proning more often, and they’ve adjusted communication with family members by making phone calls more frequently and using video chat technology.
Jo-anne says it’s all worth it. “When you help a patient on ECMO move down and out the unit, it’s very rewarding. We’re very lucky to do what we do."
More information and support
NHS England has published an ECMO service specification report with more details on how this specialist equipment works.
The RCN Critical Care and Flight Nursing Forum is a professional network which develops policy and guidance, provides specialist representation and shares best practice.