
Let’s start with the fundamental physical health ‘tasks’ - blood pressure, temperature, pulse, breathing, perhaps add in blood sugars, O2 sats, weight, tissue/skin health, bowel health. If that is the fundamentals of physical health care ‘tasks’ there isn’t one there that care homes nurses don’t do, or delegate to others to do, on a daily basis with residents. I guess it can’t be that, so we’ll have to keep on searching.
Recognition of the acutely unwell, deteriorating person is an important skill for a nurse, but is this skill limited to acute general ward nurses? Clearly the answer to this is no, this is something that a registered nurse in a care home does every day, as well as being the first responder to the deteriorating health of their residents. Unlike ward nurses, the care home nurse doesn’t have a medic in the wings ready and able to attend the person; they are required to assess the resident and consider which intervention may be required - watchful waiting, in-house treatment e.g. with medication, call the GP to attend at some point, hopefully that day or call 999 for a paramedic/ambulance response: in the meantime they are responsible for the health of that resident.
If we consider other physical health skills used in wards regularly, perhaps we’ll find the answer there - venepuncture, catheterisation, syringe pumps, IV fluids? With the exception of IV fluids, care home nurses use these other skills on a daily basis. Perhaps we have found the elusive skill that ward nurses use daily that care home nurses don’t - they use IV drips.
I can’t tell you the number of times, when I worked in the NHS, I’ve read in application forms: skills- “give out medications”. Of course, you don’t need me to tell you it can’t be this area of practice given that care home nurses can spend a significant amount of time administering medication to older adults with multiple polypharmacy needs and multiple co-morbidities, this requires knowledge of drug interactions, side effects and contra-indications. Indeed, in many of our care homes it is senior care staff that administer medications. Registered nurses are involved in reviewing medications, at a minimum of every six months along with the resident, the GP and the family. Knowledge of medication uses, interactions and side effects are a core part of the care home nurse skillset.
Perhaps it is in the mental health sphere that we will come across these vast differences in the clinical skills used regularly in the acute general ward setting that aren’t used in care homes? The assessment and interventions regarding alertness, confusion, depression, anxiety, distress, delirium - it really can’t be these either as care home nurses intervene every day to support residents who are experiencing any of these symptoms, along with dementia.
Infection Prevention & Control; is this where we are going to really understand the missing skills/knowledge of the care home nurse? Of course, in the acute hospital setting, they have teams of infection prevention and control specialists who devise and guide the ward-based nurses. So, the reality is, we find that the day-to-day clinical practice of a care home nurse isn’t that different from an acute ward nurse - both rely on specialists for advice and guidance on IPC.
Might it be in the spiritual or social sphere that ward nurses use more day-to-day clinical skills than their care home-based counterparts? I’m not clear how much time ward-based nurses spend in either the spiritual or social well-being sphere, certainly not where they use these skills more than care home nurses? Spiritual care and social well-being are key aspects of every care home nurse’s role, it is something that they spend significant time with residents getting to know their needs and wants, it’s something they excel at.
An important part of any nurse’s knowledge and skill set is to support someone to have a good death. End of life care is a critical skill and a privilege, it’s about the person, but importantly, it’s also about those around that person, it includes those who will be left behind. Anticipatory care plans, which focus on life and death are day to day part of a care home nurses’ role, it is an integral part of their skillset. Care home nurses need and uses their end-of-life care skills constantly - so I guess that can’t be the missing skills that they lose by coming to the sector.
I think we’ve established that an acute hospital ward nurse does IV infusion that a care home nurse doesn’t. Looking at the nursing role overall therefore suggests that there is no significant skill or practice difference between the hospital and the ward nurse. I suspect however, we will still have some who cling to the belief that some mythical skills will be eroded by working in a care home.
I was speaking to a student nurse a few weeks ago, yes care homes also take student nurses, and asked if she would consider care home nursing as a career choice once qualified. I respect her decision that care home nursing wouldn’t be her first choice, even though she had enjoyed her placement. I was however disappointed by her reasoning. She wanted to work somewhere with ‘more busyness’. What a shame we are teaching the following generations that being busy doing tasks is a better outcome and, in some way, more valued that spending time with the individual, to learning about them and interact at a deeper, more meaningful level. If we aren’t about people as nurses then what are we about - technicians in a caring environment or carers in a technical environment?
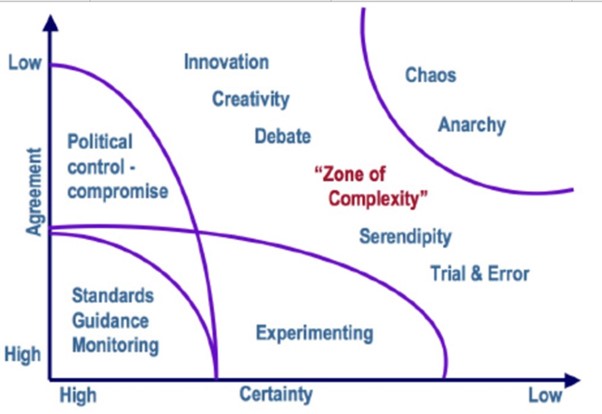
The Stacey matrix suggests the arena the care home nurse works in i.e. the impact of a lack of certainly given they don’t have the plethora of tests and medical back up the hospital nurse has, underpins the argument that it is in fact not less skilled, its differently skilled with the same foundations. It could indeed be argued that having the professional competence and confidence to work in the uncertainly is, in itself, a skill that should be both recognised and respected.
This blog isn’t saying one career choice is better than the other, it about saying that both options are legitimate, highly skilled roles that require nurses with up-to-date knowledge and decision-making skills….
…… but, next time someone says you’ll lose your skills by going into a care home, you’ll be able to challenge that ancient, handed down viewpoint with some conviction and comment on the skills, knowledge and resilience the care home nurse needs in being that senior autonomous decision maker.
Recognition of the acutely unwell, deteriorating person is an important skill for a nurse, but is this skill limited to acute general ward nurses? Clearly the answer to this is no, this is something that a registered nurse in a care home does every day, as well as being the first responder to the deteriorating health of their residents. Unlike ward nurses, the care home nurse doesn’t have a medic in the wings ready and able to attend the person; they are required to assess the resident and consider which intervention may be required - watchful waiting, in-house treatment e.g. with medication, call the GP to attend at some point, hopefully that day or call 999 for a paramedic/ambulance response: in the meantime they are responsible for the health of that resident.
If we consider other physical health skills used in wards regularly, perhaps we’ll find the answer there - venepuncture, catheterisation, syringe pumps, IV fluids? With the exception of IV fluids, care home nurses use these other skills on a daily basis. Perhaps we have found the elusive skill that ward nurses use daily that care home nurses don’t - they use IV drips.
I can’t tell you the number of times, when I worked in the NHS, I’ve read in application forms: skills- “give out medications”. Of course, you don’t need me to tell you it can’t be this area of practice given that care home nurses can spend a significant amount of time administering medication to older adults with multiple polypharmacy needs and multiple co-morbidities, this requires knowledge of drug interactions, side effects and contra-indications. Indeed, in many of our care homes it is senior care staff that administer medications. Registered nurses are involved in reviewing medications, at a minimum of every six months along with the resident, the GP and the family. Knowledge of medication uses, interactions and side effects are a core part of the care home nurse skillset.
Perhaps it is in the mental health sphere that we will come across these vast differences in the clinical skills used regularly in the acute general ward setting that aren’t used in care homes? The assessment and interventions regarding alertness, confusion, depression, anxiety, distress, delirium - it really can’t be these either as care home nurses intervene every day to support residents who are experiencing any of these symptoms, along with dementia.
Infection Prevention & Control; is this where we are going to really understand the missing skills/knowledge of the care home nurse? Of course, in the acute hospital setting, they have teams of infection prevention and control specialists who devise and guide the ward-based nurses. So, the reality is, we find that the day-to-day clinical practice of a care home nurse isn’t that different from an acute ward nurse - both rely on specialists for advice and guidance on IPC.
Might it be in the spiritual or social sphere that ward nurses use more day-to-day clinical skills than their care home-based counterparts? I’m not clear how much time ward-based nurses spend in either the spiritual or social well-being sphere, certainly not where they use these skills more than care home nurses? Spiritual care and social well-being are key aspects of every care home nurse’s role, it is something that they spend significant time with residents getting to know their needs and wants, it’s something they excel at.
An important part of any nurse’s knowledge and skill set is to support someone to have a good death. End of life care is a critical skill and a privilege, it’s about the person, but importantly, it’s also about those around that person, it includes those who will be left behind. Anticipatory care plans, which focus on life and death are day to day part of a care home nurses’ role, it is an integral part of their skillset. Care home nurses need and uses their end-of-life care skills constantly - so I guess that can’t be the missing skills that they lose by coming to the sector.
I think we’ve established that an acute hospital ward nurse does IV infusion that a care home nurse doesn’t. Looking at the nursing role overall therefore suggests that there is no significant skill or practice difference between the hospital and the ward nurse. I suspect however, we will still have some who cling to the belief that some mythical skills will be eroded by working in a care home.
I was speaking to a student nurse a few weeks ago, yes care homes also take student nurses, and asked if she would consider care home nursing as a career choice once qualified. I respect her decision that care home nursing wouldn’t be her first choice, even though she had enjoyed her placement. I was however disappointed by her reasoning. She wanted to work somewhere with ‘more busyness’. What a shame we are teaching the following generations that being busy doing tasks is a better outcome and, in some way, more valued that spending time with the individual, to learning about them and interact at a deeper, more meaningful level. If we aren’t about people as nurses then what are we about - technicians in a caring environment or carers in a technical environment?

The Stacey matrix suggests the arena the care home nurse works in i.e. the impact of a lack of certainly given they don’t have the plethora of tests and medical back up the hospital nurse has, underpins the argument that it is in fact not less skilled, its differently skilled with the same foundations. It could indeed be argued that having the professional competence and confidence to work in the uncertainly is, in itself, a skill that should be both recognised and respected.
This blog isn’t saying one career choice is better than the other, it about saying that both options are legitimate, highly skilled roles that require nurses with up-to-date knowledge and decision-making skills….
…… but, next time someone says you’ll lose your skills by going into a care home, you’ll be able to challenge that ancient, handed down viewpoint with some conviction and comment on the skills, knowledge and resilience the care home nurse needs in being that senior autonomous decision maker.








