
Clinical governance
Clinical governance covers activities that help sustain and improve high standards of patient care
Clinical governance is “a system through which NHS organisations are accountable for continuously improving the quality of their services and safeguarding high standards of care by creating an environment in which excellence in clinical care will flourish." (Scally and Donaldson 1998, p.61)
Clinical governance is an umbrella term. It covers activities that help sustain and improve high standards of patient care. Nursing staff may already be familiar with some of these activities, quality and safety improvement, for example. What is different is the effort to bind these activities together and make them more effective.
Health care organisations now have a duty to the communities they serve for maintaining the quality and safety of care. Whatever structures, systems and processes an organisation puts in place, it must be able to show evidence that standards are upheld.
The RCN aims to promote a better understanding of clinical governance with this web resource. It wants to help those working within the nursing family to become more involved with local and national quality improvement projects.
The resource describes services and support available from the RCN and these match to five key themes of clinical governance. It also shows where to find support from other agencies.
References
Scally G and Donaldson LJ (1998) Clinical governance and the drive for quality improvement in the new NHS in England. British Medical Journal 317(7150) 4 July pp.61-65.
This diagram illustrates the five interconnected key themes that form a framework to look closely at how to improve the quality of care.
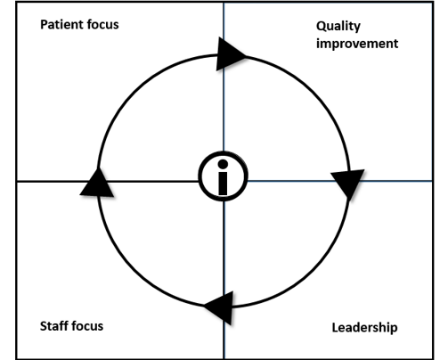
Five key themes appear repeatedly in policy documents about healthcare quality:
- Patient focus - how services are based on patient needs
- Information focus - how information is used
- Quality improvement - how standards are reviewed and attained
- Staff focus- how staff are developed
- Leadership - how improvement efforts are planned.
These five themes are interconnected. Together they provide a framework to look more closely at those things that make the difference to quality of care.
Public inquiries and investigations into poor care quality usually show that multiple dimensions of care are involved.
Sir Robert Francis, author of the Mid Staffordshire Inquiry report (Francis 2013), described the breakdown of fundamental clinical governance practices:
- No systems in place for systemic appraisals of clinical quality or of staff
- Information gathering was “inept” and coding “dreadful”
- Staff were not “gripped” by the importance of clinical governance
- No culture of self analysis
- Little analysis of complaints or incidents
- The risk register was not kept up to date.
The RCN has developed this resource to support those wanting a deeper understanding of these themes and what can be done to make a positive impact on patient care.
References
Francis R (2013). Mid Staffordshire NHS Trust Public Inquiry
A key part of patient centred care is allowing people to engage in their own health and help design health systems. Learn about the four areas where patients are getting involved.
Service design – the care environment can influence people’s experience of services. Changing aspects of the service can improve dignity or provide people with better control over a situation. Patients, families, carers and staff can use a design method such as Experience Based Co-design to achieve better care. Dr Caroline Shuldham, Director of Nursing, introduced this method at the Royal Brompton and Harefield NHS Trust to improve ITU and lung cancer services.
Process design – we can improve care by looking at processes such as drug rounds, mealtimes, home visits. This may mean reviewing roles, data use or the sequence in which actions occur. The RCN published a joint report with the RCP about addressing shortcomings of traditional ward rounds. Structured interdisciplinary bedside rounds offer an alternative approach (RCP, RCN 2012).
Feedback/feedforward – systems need continuous feedback in order adjust how they perform. Michelle McLoughlin, Birmingham Children’s Hospital Chief Nurse, introduced an app that enables families to give feedback. Their anonymous comments go directly to the manager in charge.
Participatory health and patient activation – participatory health refers to a person provider partnership based on mutually acknowledged expertise. Patient activation describes the knowledge, skills and confidence a person has in managing their own health (Hibberd and Gilburt 2014). A recent study (Armstrong et al 2015) shows how NHS projects promoted this e.g. NHS Somerset CCG working with people on diabetes self management and those living with long term conditions.
References
Armstrong N et al (2015) Independent evaluation of the feasibility of using the Patient Activation Measure in the NHS in England Early findings. NHS England.
Hibberd J, Gilburt H (2014) Supporting people to manage their health. An introduction to patient activation. London: King’s Fund.
Royal College of Physicians, Royal College of Nursing (2012) Ward rounds in medicine: principles for best practice. London: RCP.
RCN support
Principles of Nursing Practice. The Principles of Nursing Practice describe what everyone can expect from nursing practice whether colleagues, patient, their families or carers. They provide a framework for quality improvement initiatives. Principle A focusses on dignity, equality and diversity, and humanity. Principle D encompasses themes of advocacy, empowerment, patient-centred care, and patient involvement in their care.
Safeguarding. Safeguarding is relevant to all of nursing practice, in all settings, whether with children or adults. As a nurse, midwife, health visitor or HCA you are responsible for safeguarding those in your care and you must respond to any safeguarding concerns. The RCN has published safeguarding guidance for adults and children and young people.
Looking for articles and books on this topic?
The RCN library and heritage services provides books, e-books and e-journals on this topic.
- Timely – reducing waits and delays
- Effective - providing services based on evidence and which produce a clear benefit.
- Person-centred - establishing a partnership between practitioners and patients to ensure care respects patients’ needs and preferences.
- Efficient – avoiding waste
- Equitable - providing care that does not vary in quality because of a person’s characteristics.
- Safe - avoiding harm to patients from care that is intended to help them
understanding the problem, with a particular emphasis on what the data tell you
understanding the processes and systems within the organisation – particularly the patient pathway – and whether these can be simplified
analysing the demand, capacity and flow of the service
choosing the tools to bring about change, including leadership and clinical engagement, skills development, and staff and patient participation – evaluating and measuring the impact of a change. (Health Foundation 2013).
References
HQIP (2015). Guide to quality improvement methods.
Health Foundation (2013) Quality Improvement Made Simple.
RCN support
RCN Principles of Nursing Practice. The Principles describe what everyone can expect from nursing practice, whether colleagues, patients, their families or carers and provide a framework for care and quality improvement. This resource introduces the Principles and describes how they relate to other publications about the quality of nursing care. Principle C focuses on the safety of all people (patients, visitors and staff), the environment, organisational health and safety, management of risk, and clinical safety.Patient safety and human factors. An online resource which introduces a broad range of activities relating to patient safety and human factors. The resource signposts further resources and support available from the RCN, and provides an overview of the active patient agenda being pursued across the United Kingdom.
Looking for articles and books on this topic?
The RCN library and heritage services provides books, e-books and e-journals on this topic.
The RCN believes that workplaces can improve the health and wellbeing of nursing staff. Healthier working environments can improve patient outcomes.
A report commissioned by NHS England (Dawson, 2018) shows the strong links between staff experiences and the care provided to the patient.
The form of support staff receive from supervisors and others, and the level of staff engagement have an impact on care. When staff are positive about levels of support this can lead to improved patient satisfaction, health outcomes, and ratings of quality of care, as well as reduced staff absenteeism and turnover. Aiken (2014) in the RN4CAST study reported that improvements in hospital working environments may be a cost-effective means to improving safety and quality in hospital care.
The RCN supports the health, safety and wellbeing of RCN members across the UK, see: Health, safety and wellbeing.
References
Aiken (2012) Patient safety, satisfaction, and quality of hospital care: cross sectional surveys of nurses and patients in 12 countries in Europe and the United States. BMJ 344:e1717.
Dawson (2018) Links between NHS staff experience and patient satisfaction: Analysis of surveys from 2014 and 2015.
RCN support
First Steps for health care assistants. First Steps for health care assistants (HCAs) is a quality-assured, online learning resource developed by the RCN to support health care support workers (HCSWs) with their induction and early learning.
Get help from the RCN. As an RCN member, you can access our online advice pages for help on a range of issues or contact us for confidential advice and support on workplace and legal issues, careers, immigration, money worries and more.
Health, safety and wellbeing. The RCN supports the health, safety and wellbeing of RCN members across the UK, by campaigning and influencing for sustained improvements to the working environment of our members and ensure their health, safety and wellbeing is seen as a priority by employers, regulators, and the UK governments.
NMC Revalidation. The NMC is in the process of piloting a proposed revalidation model; a process for NMC registrants to show they remain fit to practise and remain on the NMC register. The Royal College of Nursing wishes to support registrants with this process as it develops, by producing and developing this online resource that meets the needs of all nurses and midwives and supports the information that the NMC is providing.
RCN Principles of Nursing Practice. The Principles describe what everyone can expect from nursing practice, whether colleagues, patients, their families or carers and provide a framework for care and quality improvement. This resource introduces the Principles and describes how they relate to other publications about the quality of nursing care. Principle F focuses on evidence-based practice, technical skills, education, training and clinical reasoning. Principle G encompasses themes of care and treatment, multi-disciplinary and multi-agency working, and co-ordination, integration and continuity of care.
Looking for articles and books on this topic?
The RCN library and heritage services provides books, e-books and e-journals on this topic.
Leaders are critical in shaping organisational culture.
How can leaders ensure that the workplace supports high quality, safe and compassionate health care? How are leadership behaviours, strategies and qualities developed? The King's Fund review provides an insight into how leadership works. The leadership task is to ensure direction, alignment and commitment within teams and organisations.
Nurses prefer managers who are participative, facilitative and emotionally intelligent. Leadership styles contribute to team cohesion, lower stress, and higher empowerment and self-efficacy. Leadership is a predictor of quality outcomes in health care settings. Authentic leaders offer good role models consistent with values and vision for health care. They offer individualised consideration of staff, provide motivation and stimulate of creativity and innovation.
Collective leadership is a more recent area of interest. It reflects the assumption that acts of leadership should come from anybody, not only those in formal positions of authority. Finally there has been much investment in leadership programmes. But the evidence base for leadership interventions remains unclear.
References
King's Fund (2015) Leadership and leadership development in health care. The evidence base
RCN support
Executive Nurse Network. The Executive Nurse Network is a support network of senior nurses. This network is for Directors of Nursing, Deputies or Assistants who may or may not have board level responsibility. The network is also on Twitter: @rcnenn
Clinical and Political leadership programmes. Quality leadership is vital to your organisation and to patient safety. Utilising our knowledge and expertise, RCN’s leadership programmes will cultivate leadership skills and shape participants as future leaders.
Nurses in Management and Leadership Forum. These pages will keep you up to date with what is going on in health and social care by bringing you news and links to keep you abreast of developments in the RCN and the UK. Most importantly they allow you to share your experiences and developments directly with other RCN members.
RCN Principles of Nursing Practice. The Principles describe what everyone can expect from nursing practice, whether colleagues, patients, their families or carers and provide a framework for care and quality improvement. This resource introduces the Principles and describes how they relate to other publications about the quality of nursing care. Principle H encompasses themes of leadership contributing to an open and responsive culture.
Looking for articles and books on this topic?
The RCN Library and Heritage services provides books, e-books and e-journals on this topic.
The third wave is about the complete digitization of whole services. With this comes the possibility of new ways of working and living that will impact on everyone. What will this look like for healthcare?
Personalised or precision medicine: is defined as the application of emergent technologies (such as genomics) to better manage patients’ health and target therapies to achieve the best outcomes in the management of a patient’s disease or predisposition to disease. Precision medicine should both improve patient outcomes and deliver benefits to the health service, including reducing the cost of ineffective treatment and multiple tests.
Electronic health records (EHRs): The integration of health and health and social care to support joined up patient pathways requires shared records.
Mobile technology: advances in smart phone design has meant that patients and carers can research information online, study treatment options and share experiences. From a health provider viewpoint the benefits can mean minimising avoidable service use, reducing paperwork and increasing patient face time (Deloitte 2015).
Alongside digital developments are what have been called social innovations (Nesta 2015) – innovations that harness the power people (patients, carers, communities and citizens) to improve health. Both digital technologies and social innovations are shaping health care now and in years to come.
References
Biesdorf S, Niedermann F (2014) Healthcare’s digital future. McKinsey & Company.
Deloitte Centre for Health Innovations (2015). Connected health. How digital technology is transforming health and social care (PDF).
Nesta (2015) The NHS in 2030. A vision of people-powered, knowledge-powered health system.
National programmes / strategies
Department of Health: Digital-first public health: Public Health England's digital strategy (2017). This document explains how Public Health England (PHE) will make best use of digital to meet the needs of our users and fulfill our remit to protect and promote health and reduce inequalities.
Department of Health: The power of information (2012). This strategy sets a ten-year framework for transforming information for health and care. It aims to harness information and new technologies to achieve higher quality care and improve outcomes for patients and service users. Underpinned by the Health and Social Care Act 2012, it covers public health, healthcare and social care in adult and children’s services in England. The vision set out in the strategy is that "patients are in control of the information they need to improve their health and wellbeing and NHS information systems are designed to support clinicians and other front-line staff to deliver safe, high quality care to their patients".
NHS England: Leading Change, Adding Value: A framework for nursing, midwifery and care staff (2016). As part of 10 commitments to delivering and improving care, NHS England encourages health care professionals to champion the use of technology and informatics to improve practice, address unwarranted variations and enhance outcomes.
NHS Five Year Forward View (2014). The NHS Five Year Forward View sets out a new shared vision for the future of the NHS based around the new models of care. It has been developed by the partner organisations that deliver and oversee health and care services including Care Quality Commission, Public Health England and NHS Improvement. Patient groups, clinicians and independent experts have also provided their advice to create a collective view of how the health service needs to change over the next five years if it is to close the widening gaps in the health of the population, quality of care and the funding of services.
Northern Ireland Department of Health. Digital Strategy 2022 - 2030. Making lives better for the people of Northern Ireland, using digital to transform the way health, care and well-being services are delivered.
Northern Ireland: eHealth and Care Strategy. This eHealth and Care Strategy sets out a range of measures for the increased use of digital technologies to support the delivery of health and care services between now and 2020. The Strategy is built around the key objectives of supporting people, sharing information, using information and analytics, fostering innovation, modernising the eHealth infrastructure and ensuring good governance.
Scottish Government. Scotland's Digital Health and Care Strategy: enabling, connecting and empowering (2018). This strategy shows how Scotland will use technology to reshape and improve services, support person-centred care, and improve outcomes.
Scotland: A digital strategy for Scotland 2017 and beyond: a view from the professions (PDF). This digital strategy sets out the changes that need to take place within health care services to improve patient care and health and wellbeing outcomes across Scotland.
Wales: Population health in a digital age The use of digital technology to support and monitor health in Wales (2019) (PDF). This report looks at how technology is used to support and monitor health in
Wales: Digital Inclusion Guide for Health and Care in Wales (2019) (PDF). This report is aimed at health and social care organisations and includes practical advice on how to support digital inclusion at a local level.
RCN support
Digital Nursing Forum: this is a forum for nurses who are working or interested in the use (collecting, recording, storing, retrieving and sharing) of clinical data and information for the advancement of patient care and nursing. It aims to promote, develop and integrate an awareness of eHealth and health informatics into every area of professional nursing practice, research and education.
RCN Principles of Nursing Practice. The Principles describe what everyone can expect from nursing practice, whether colleagues, patients, their families or carers and provide a framework for care and quality improvement. This resource introduces the Principles and describes how they relate to other publications about the quality of nursing care. Principle E focuses on communication, handling feedback, record keeping, reporting and monitoring.
Looking for articles and books on this topic?
The RCN library and heritage services provides books, e-books and e-journals on this topic.
Together, we can build a better future for nursing







