
Model of reflection for prison nursing
Reflection on and in practice is promoted in nursing, with numerous models of reflection and tools available for people to use to help guide their thinking and reflection.
Experience suggests that when left to reflect on their practice, nurses will often resort to reflecting on negative experiences, placing themselves at the centre of the reflection and focussing on their own perceived deficits and failures, with very little consideration of the impact of the environment and the human factors that may have been of significance.
Given the significant impact of the prison environment and culture on nursing practice, this model of reflection encourages prison nurses to consider the human factors at play in any practice experience they reflect on.
The discipline of Human Factors (HF) is defined by Karwowski et al (2025:361) as ‘the scientific discipline concerned with the understanding of the interactions between humans and other elements of a system, and a profession that applies theory, principles, data and methods to design in order to optimise human wellbeing and overall system performance’.
It is this understanding of the interactions between humans and other elements of a system that we suggest makes HF a useful lens through which to look at nursing practice in prison, given that the prison environment and culture pose unique challenges for prison nurses.
These unique challenges are often because of the organisational culture and environment, where the security apparatus which views health care and security as competing priorities. Ramluggan et al (2019:366) note that the prison environment is ‘designed for incapacitation’ where ‘procedural security measures are imperative to the credibility of the prison system to safely keep prisoners in custody to maintain public safety but create a rigidly structured and regimented environment which closely regulates prisoners lives and equally, the daily lives of prison officers and nurses’.
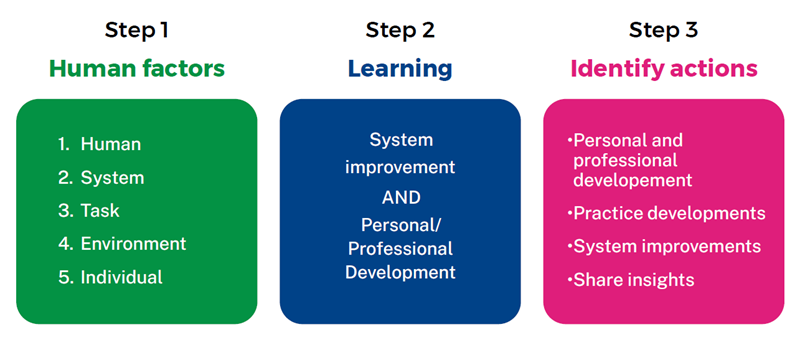
This model of reflection has three stages:
- Exploration of Human Factors (human interactions and self/individual factors).
- Consideration of learning, both individual and system.
- Next steps/actions which consider both personal and systemic levels.
Step 1: Human factors
Human–human Interaction (anyone involved including both patients and staff)
- Team dynamics, conflict, leadership, hierarchy, power/status, incivility/civility, compassion fatigue, malignant alienation, understanding, verbal/non-verbal/written communication, substance use, appropriate language.
Human–system interaction (consider areas such as information systems, policies, practices)
- Organisational flow, system usability (intuitive and accessible), system culture impacting on action, layout, influence of automation, system ambiguities, policies/SOPs, system impact on both patients and staff.
Human–Task Interaction (includes equipment)
- Does the equipment work, is it clean/accessible/well-resourced/properly stored, familiarity with the task/equipment, cognitive load/mental effort, is it matched to capability, do we know the policy/SOP, what does the task demand of me.
Human–environment interaction
- Physical environment, location of activity, infrastructure, security measures, atmosphere (temperature, humidity, smell, lighting, noise, cleanliness etc), interruptions, cultural norms/expectations.
Individual/self/personal considerations
- How were you feeling? What was happening in your life? How is morale? How confident/motivated/enthusiastic were you feeling?
- Cognitive factors: attention, memory, perception, decision making, mental workload.
- Physical factors: strength and stamina, vision, hearing, touch, coordination, dexterity, reaction time, fatigue, hunger/thirst.
- Psychological factors: Stress and anxiety, emotional state, motivation, personality traits (risk tolerance, conscientiousness), mental health.
- Experiential factors: your own training and experience, knowledge and expertise related to the event.
Step 2: Learning
- System improvement, and
- Personal/professional development.
Step 3: Next steps–identify actions
- Personal and professional development
- Practice developments
- System improvement
- Share insights.
Factors to consider during reflection (adapted from Rosenorn-Lanng R, 2014).
References
- Karwowski W, Salvendy G, Endsley M, Rouse W, Salmon P, Stanney K, Thatcher A, Andre T, Yang J, Ayaz H, Cakir A, Duffy V, Drury C, Gao Q, Guo Y, Hancock P, Marras W, Rau P, Sawyer B and Stanton N (2025) Grand challenges for human factors and ergonomics, Theoretical issues in Ergonomics Science, 26(4), 361-456.
- Rosenorn-Lanng R (2014) Human Factors in Healthcare: Level One, Oxford: OU Press.
- Ramluggan P, Nathoo S, Jackson D and Usher K (2019) Does compassion matter in custodial care? International Journal of Mental Health Nursing, 28, 365-368.
* This model of reflection was developed throughout 2025 as part of a funded project with Central North West London NHS Foundation Trust to enable and promote professional practice in prison healthcare settings.





