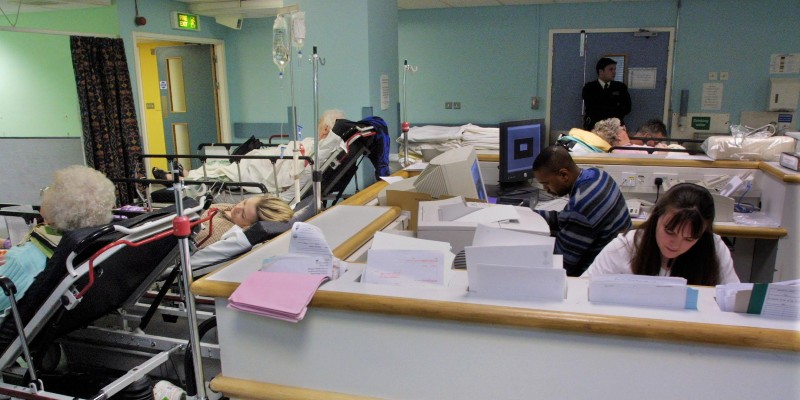
More than five hundred specialist A&E nurses shared their experiences of overcrowded hospitals ahead of RCN Congress, which begins today (15 May) in Brighton.
Delegates at the annual conference will discuss the impact of “corridor care” and the “moral injury and distress for nursing staff, knowing they’re providing suboptimal care to patients.”
The survey of emergency care nurses reveals more than eight in 10 say treatment in non-designated clinical areas, including store rooms, has increased since the beginning of last year.
Over nine in 10 raised concerns that patients may be receiving unsafe care, and patient dignity, privacy and confidentiality is compromised. More than six in 10 added that the situation leads to fears of being struck off the nursing register or a court case as a result of patient harm.
Two thirds have faced increased violence or aggression from frustrated patients and relatives, while a third said they didn’t feel comfortable to raise concerns about the impact of providing care in inappropriate settings.
Free-text responses saw nursing staff describe feeling “broken” and “suicidal”, corridor treatment being “degrading” for patients, and nurses leaving the NHS as a consequence, including after a death in the corridor.
Corridor care has become more common due to increased demand on hospitals because of a lack of GP appointments. Hospitals are also unable to discharge patients because of a lack of community care provision. Bed capacity runs at dangerous levels and patients in emergency departments can’t be moved to wards. As a result, emergency care staff provide care in inappropriate settings to cope with high numbers of patients.
RCN General Secretary & Chief Executive Pat Cullen said: “This bleak picture comes from right across the NHS. Patients backed-up through emergency departments is a stark sign of a health and care system grinding to a halt. A corridor is no place to die and no place to work either.
“When ministers fail to grip this situation, they allow patients to pay a high price and nursing staff to work in fear, professionally compromised. Governments must urgently plan and invest to reverse this new trend.”
Ahead of the debate at RCN Congress, an emergency care nurse said: “Caring for patients in corridors is destroying staff morale. When you walk into the department and see 15-20 people in the queue, day in day out – you lose any hope it’s going to be a good shift.
“We care for patients the best we can, but something happens every day. I’ve dealt with almost every situation I can imagine in the queue. We’ve had to fit call bells and crash buzzers after people have had cardiac arrests in a corridor.
“Patients who are incontinent need pads changing but there’s no space or privacy to change them. Patients and their relatives can sometimes be physically or verbally aggressive towards us because they’re rightly scared and horrified about the setting they’re being treated in – some are then arrested or removed by security. There are delays to medication. The list goes on.
“Having to care for patients in this way makes you feel you’re a terrible nurse. Sadly, I have become desensitised to it as I’ve been dealing with it for so long. But unless something is done, we will continue to lose brilliant nurses who are getting to breaking point.”
The RCN has produced a range of resources for nurses working under unsustainable pressures.





